Much has happened since my last blog post about Gareth, so I'll try to be thorough and concise.
--
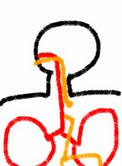
Gareth went in for surgery on Thursday morning around 9:15. The purpose of the surgery was two-fold: to sever the connection between the esophagus and trachea and to attach the two disconnected portions of Gareth's esophagus. Cliff drew some pictures of this on his i-pod touch to illustrate for our family. They are below - the first one is how Gareth's esophagus was originally, and the second is how it normally looks (and looks now after surgery). Notice the top portion of the esophagus ended in a pouch and the bottom portion connected to the trachea.
Here was the difficulty - there was no way for the surgeons to know if Gareth had enough esophageal tissue to connect the separated portions until they were already in surgery. Thus, if there wasn't enough, they would only sever the connection between the esophagus and trachea and then do a procedure to begin the stretching of the esophagus. This would prolong our stay in the NICU, as Gareth would still be unable to eat and would have to wait for another surgery to connect the two ends - probably a month later. So, you can see how stressed we were when Gareth went into surgery; we wouldn't know what our future held until the surgeon came out afterwards.
At about 1:15pm, the surgeon called us into a conference room and gave us the wonderful news that they'd been able to connect the esophageal ends with no difficulty. He said, in fact, that our son has a great anatomy. That wasn't a joking phrase either - we'd only recently discovered that Gareth's condition is part of a syndrome that usually includes heart problems, renal problems, spinal malformations, missing bones or hand digits and even rectal problems. Fortunately, Gareth had none of these associated problems - we've heard our doctors on rounds say things like "oh, Gareth...he'll be fine. He only had one problem!"
So what happens next?
Well...blessedly...we just wait. Gareth's esophagus has to heal before we can do any oral feedings (whether by bottle or breast), so the surgical team will do a "dye test" on this coming Thursday to see if there are any "leaks" at the surgical site. If that goes well (and by well I mean, no leaks), then we can do oral feedings, his chest tube will come out and probably his central line. At that point, the goal will be to successfully feed, burp and soil diapers and then we'll be able to go home. That could be next weekend or it could be a couple of days afterwards, it's really up to the doctors. When we know more, we'll let you know.
Now we're just sitting around watching him improve. He is no longer receiving any antibiotics or pain medication, he has increasing amounts of breast-milk fed through his NG tube (a tube that goes directly to his stomach), his hep-lock ports in his hand and foot have been removed, his catheter is out as is his ventilator, he has stopped receiving photo-therapy for jaundice, and he can be touched and handled without gloves or protective gear. We still can't hold him (b/c of the chest tube), but that day is coming.
This last week has been at times glorious and horrific, terrifying and exhilarating. But through it all, we are thankful to you for all your kind words and prayers. It has been moving to stand by our son's bedside and know that the community of saints and the spirit of God is surrounding us.


No comments:
Post a Comment